
The goal was to include all the pregnant women who met the inclusion criteria. Patients in whom ultrasound imaging could not be performed were excluded. All pregnant women over 18 years of age receiving care during the three years of the study and who met the following criteria were included: a) 12 weeks or more of gestational age and b) a positive history of uterine surgery (cesarean section, myomectomy or curettage) or placenta in anterior location, low or praevia (total or partial). This institution is the referral centre for the public hospital network in the northeastern region of Colombia and provides services mainly to low-income patients affiliated to the contributive insurance regime of the Colombian social security system. Diagnostic test accuracy assessment study in pregnant women seen for prenatal care and who ended their pregnancies between 20 at Hospital Universitario de Santander (Santander University Hospital - HUS). Given the variability of accuracy indicators of 2D ultrasound for the diagnosis of placenta accreta, the potential usefulness of adding Doppler to the prenatal study, and the scarcity of research conducted in this country, the objective of this study was to assess the diagnostic performance of combining obstetric 2D ultrasound plus Doppler for the diagnosis of this condition in high-risk women in a Level III perinatal care centre in the city of Bucaramanga, Colombia.ĭesign and population. On the other hand, there are reports that describe good accuracy of Doppler ultrasound in placenta accreta 34. In Colombia, there are three reports related to ultrasound diagnosis of placenta accreta, all of them with limitations in terms of patient number and selection and the type of information provided 31 - 33. These variations may be partly explained by the population studied, by the fact that it is operator-dependent 30 and by the ultrasonographic criteria used. The sensitivity of 2D ultrasound described in the literature ranges between 86% and 100%, while specificity is around 66% to 98% 26 - 29. Moreover, no significant improvement in outcomes has been found with the use of this imaging modality in placenta accreta pregnancies 25. However, it has high cost, not readily available, and some patients may feel claustrophobic 23, 24. 
Magnetic resonance imaging (MRI) is used to assess posterior placenta accreta or when invasion of adjacent organs is suspected. In patients with risk factors, it is advisable to assess placental implantation after 12 weeks in the office using 2D ultrasound and Doppler or nuclear magnetic resonance in order to look for signs that may suggest placenta accreta 21, 22. Given the threat posed by placenta accreta, the best approach is prenatal diagnosis 3, 10 - 12, 15 in order to ensure timely referral to centres with the human and technical resources for adequate delivery care and response to potential complications such as massive bleeding, thus reducing the risk of maternal death 9, 16 - 20. Another risk factor is placenta praevia or low-insertion placenta (placental tissue that extends over or close to the internal os), which may occur in up to 9.3% of pregnancies 3, 1-3% of which are accompanied by placenta accreta 14, 15. 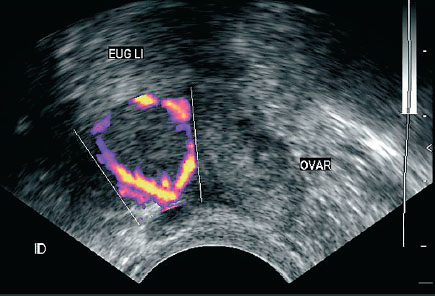
Women with uterine scars due to surgical procedures such as cesarean section (c-section) or myomectomy have a higher risk of placenta accreta, and this explains why the incidence has increased ten-fold over the past three decades, clearly in association with the growing number of cesarean sections 10 - 13. Placenta accreta impairs or hinders normal placental detachment 6, 7, constituting a relevant problem, because although it occurs in 0.1-0.3% of pregnancies 2, up to 80% of patients develop massive bleeding due to abnormal placental detachment 8, creating a considerable risk of maternal morbidity and mortality 9. Three variants of placenta accreta have been proposed according to the degree of trophoblast invasion: accreta, increta and percreta 5. Placenta accreta is the abnormal insertion of the placenta to the uterine wall beyond the fibrin layer or Nitabuch layer 1, secondary to total or partial decidual absence 2, with trophoblast villi penetration into the myometrium and even into the serosa or adjacent organs 3, 4.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
